The Shift in Justice: How Legal Changes Reflect Society’s Moral Reckoning
In recent months, a landmark judicial decision by the UK Supreme Court has sent ripples through the fabric of families, communities, and public health systems. The court’s ruling, which allows children who suffer catastrophic injuries at birth to claim damages for future earnings, marks a profound cultural shift—away from the traditional legal stance that limited such claims—highlighting society’s evolving criteria for justice and moral accountability. The implications of this decision reflect not only a legal milestone but also expose the underlying societal tensions around #healthcare responsibility and social justice.
Lives Changed, Justice Redefined
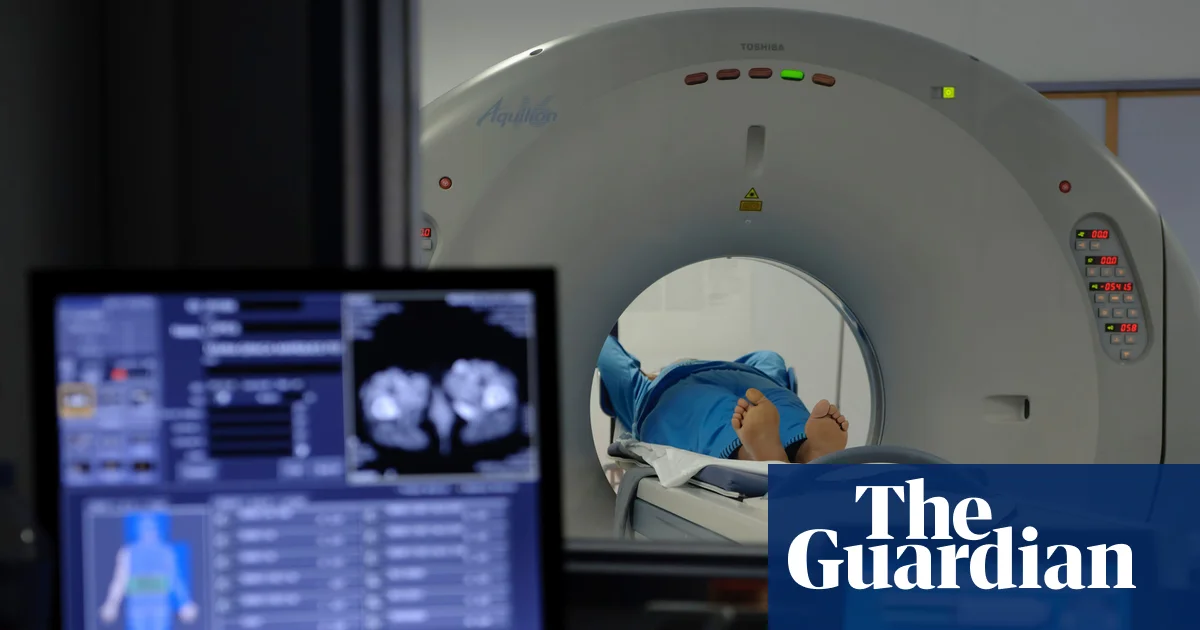
This ruling comes at a time when the NHS faces escalating financial strains, with liabilities soaring to over £60 billion largely due to medical negligence during childbirth. Families like that of a girl known as CCC, who endured irreversible brain damage due to medical errors, embody the human cost behind the mounting figures. Her family secured a substantial settlement in 2015 but were denied compensation for lost years, a gap now addressed by the recent legal decision. Sociologists like Anthony Giddens might say that this judicial shift signifies a societal move towards recognizing the moral obligation to uphold the rights of vulnerable children—an acknowledgment that justice for the injured extends beyond immediate damages to encompass their entire life trajectory.
Social Challenges and Communities at Crossroads
- Education and Family: The ruling underscores the importance of education for families about legal rights and healthcare responsibilities, highlighting the need for societal support systems to adapt in tandem with legal reforms. It presents a challenge: how can communities ensure that families, especially those in vulnerable demographics, are equipped with the resources and knowledge to navigate these complex issues?
- Health System and Policy: The NHS’s increasing liabilities raise questions about preventative care and systemic reform. Social commentators argue that better investment in prenatal care, staff training, and accountability mechanisms could reduce incidents of negligence. The debate now centers on whether policy can keep pace with societal expectations of justice, or if systemic failures will continue to scar generations.
- Broader Societal Impact: The societal moral fabric is tested as the line between public responsibility and individual rights becomes clearer. This legal evolution could set precedents affecting future cases, ultimately challenging the notion of collective social justice versus institutional liabilities.
As social thinkers like Hannah Arendt have noted, a society’s moral character is defined by how it cares for its most vulnerable. This decision prompts a reflection on whether justice truly operates as a societal equalizer or if it exacerbates disparities in access and awareness.
Reflections on Society’s Journey
The recent landmark ruling embodies a society on the cusp—struggling to reconcile the moral imperatives of compassion with the realities of systemic failure. Beneath the legal language lies a poignant reminder that every societal law is rooted in moral choices. The hope remains that through ongoing dialogue and reform, communities can forge a future where justice no longer leaves behind those most in need, advocating for families damaged by preventable tragedy and reaffirming societal values of accountability, compassion, and resilience. Society’s greatest challenge is transforming this legal milestone into a catalyst for meaningful social change, fostering a community where learning from past errors leads us toward a more just and humane future—a future where society, like a caring parent, must hold itself accountable for every child’s right to a fair start.